My cancer
I have prostate cancer and will begin treatment in January.
I wanted to share my experience for several reasons. First, if you have a prostate, you might benefit from hearing somebody else’s experience — since you may find yourself in the same boat I’m now in. Second, I made my decisions in consultation with my doctors and based on science — that’s how I roll, and you might find it useful to see how I applied that type of thinking in a high-stakes situation. And third, I feel like sharing what just happened with my followers.
And fourth, I guess, I get to share a lot of cool stuff I learned about word origins and fancy math computations.
Three warnings before I go on.
- Don’t take my story as medical advice: talk to your own doctor.
- If you’re squeamish about things like bladders and male genitals, you might not enjoy this account very much. I don’t get into disgusting detail, but hey, we’re talking about a body part here that’s usually considered private and some people don’t like to think about that. Fair warning, nearly every link in this post takes you to a diagram of parts of the body that most men are sensitive about, in situations that most people would rather not think about. If that’s you, skip this post and read about, say, my amusing travails getting companies to actually pay me.
- Having made a decision, I don’t now want to hear your medical advice for me. My doctors have all my test results and scans and I’ve talked to several to get different opinions so I can make the wisest possible decision. Your own experience with cancer is highly relevant to you, but not applicable to me in my specific situation. Don’t email me your medical advice, and don’t post it in comments either. Your sympathy is another matter — I’ll gladly take that.
What’s the deal with the prostate?
The prostate gland is a little lump of tissue about the size of a plum that’s situated right behind your male reproductive organs. According to my friend who is a word origins expert, Jess Zafarris, author of Once Upon a Word, prostate comes from the Greek prostatēs, meaning leader, ruler, or guardian, or more literally, “one standing in front,” because it stands in front of the bladder.
(I always wondered about the similar word prostrate, but that comes from Latin meaning to lay down [before someone]. So prostrate = laying down, prostate = standing in front. Don’t confuse ’em or you’ll look like quite the fool talking about prostrate cancer, a dreaded disease of people who grovel.)
In any case, as with many reproductive parts of the human body, once you’re done reproducing, your prostate is “out of warranty” from an evolutionary perspective, so your genes don’t care if it malfunctions. An amazing one out of eight men will be diagnosed with prostate cancer at some point, and it is the second leading cause of cancer death in American men, behind lung cancer.
While that is scary, prostate cancer is a very slow-growing cancer. Lots of older men get it, but it’s a truism in the field that more men die with prostate cancer than of prostate cancer. How can that be? It’s because while a whole lot of men get prostate cancer, those men tend to be fairly old, and they get even older and die of something else before the slow-moving prostate cancer gets out of control.
How do you find out if you have prostate cancer?
If you have a prostate that’s causing problems, the first thing that you probably notice is that you get up and go to the bathroom several times a night, a condition called nocturia (which is apparently from the Greek for “have to pee at night”). That’s because your prostate is pressing on your bladder. But lots of guys have that annoyance and don’t have cancer — it’s just the symptom most likely to get your doctor’s attention.
If you have that symptom, as I did, they do a blood test called PSA (prostate-specific antigen) test, which tests for a chemical that cancerous prostate cells secrete. But it’s a maddeningly imprecise test. If you score above 4 ng/mL, the doctors get suspicious. The higher you get, the more suspicious they get. But only 25% of people with high PSAs turn out to have cancer detected by a biopsy. The other test they do is the one where the doctor puts on a rubber glove and . . . well, I won’t go too much further into detail about that, everybody over 45 with a prostate has experienced that test, but let’s just say it’s also typically not all that precise for diagnosing anything.
My PSA score was 9, which perked up the doctors right away (I’ve always gotten outstanding scores on tests and this was no exception). Unfortunately for me, I got this information just as I was moving to Portland, Maine in the fall of 2021. I pathetically begged a doctor friend of mine who teaches family medicine at the Tufts Medical School to find me a good doctor in Maine, he did, and that primary-care doctor quickly referred me to a urologist in Maine.
Prostate biopsies and “active surveillance”
I was at risk because of a family history of prostate cancer. Due to that and the high PSA score, they scheduled a more accurate diagnostic test: a prostate biopsy. You may wonder how in heck they can take core samples of a gland that’s stuck up behind your private parts. It’s unpleasant — there’s a diagram here, but I don’t recommend perusing it unless you really want to know. One friend told me it was the most painful thing he’d ever experienced, but my personal experience was, hey, no big deal, sort of like getting shot with a staple gun in places you’d really rather not get shot with a staple gun. You will have to take antibiotics before the test, which has some annoying side effects.
After the biopsy, they look to see how many core samples have cancer and what level of cancer it is (that is, how disordered the cells look under a microscope). Each core gets a “Gleason score” on a 10-point scale.
In my case, a few of the cores were positive and the Gleason score was 6, which is the lowest grade that is actually cancer.
The tricky thing about prostate cancer is that because it grows so slowly, the best strategy is often to just keep an eye on it rather than any actual treatment. This strategy used to be called “watchful waiting” and has been renamed to “active surveillance” (because men would rather participate in espionage than waiting, I guess). That means you and your doctors will do regular tests but won’t initiate any treatment unless there are signs that the cancer is getting worse, because the treatment is more of a risk than the cancer is. In many cases, this means you can just go about the rest of your life and ignore it (except for getting up to pee in the night, of course).
Based on the low Gleason scores in just a few cores, I went into active surveillance, with a plan to check it again in a year or so.
From surveillance to treatment
In my case, active surveillance meant that a year after the previous biopsy, I had a pelvic MRI. This is partly to look for abnormalities and partly to allow the urologist to aim more precisely in the next biopsy.
Sure enough, the MRI showed some lesions that didn’t look the way they should. So I had the second biopsy in November of this year — which was no more or less unpleasant than the previous one.
I thought I was in fine shape, since once again the cores were a Gleason score of 6. And when I met with my urologist, he said, “I think we’re done with the watching.” For a minute I thought he meant “no more active surveillance.” But as he continued speaking I found out what he really meant: time to start treating the cancer. Because although the Gleason score hadn’t increased, there was cancer in more cores, there were the abnormalities in the MRI (some of which were actually past the edge of the prostate), and the doctor had felt a lesion in his exam.
There are three basic ways to treat prostate cancer.
- You can get your whole prostate removed surgically. This is called a radical prostatectomy. Since both your urine and your semen go right through a duct within the prostate that has to be reconnected during the surgery, this surgery has some unpleasant side effects. It’s robotic surgery and minimally invasive, but it’s still surgery. It has a high cure rate but if the cancer has escaped the prostate it still might not work.
- You can have radioactive “seeds” implanted in your prostate to nuke the cancer. This is called brachytherapy. (brachy is greek for “short” or “nearby” and has nothing to do with achy-breaky hearts). I know people who’ve had this and they’re still walking around just fine.
- You can get external beam radiation. That is, they shoot targeted radiation at your body in the places where the abnormal cancer cells appear to be.
These therapies sometimes also include hormones that basically stop your testosterone, but as you can imagine, while this stops the cancer from growing, it also interferes with other elements of your male hormones in ways that have unwanted side effects, so it’s not really a long-term solution.
In my case, the prediction is that the external beam radiation has an 85% chance of curing the cancer (I asked what that actually means, and in this case, a cure means you eventually die of something other than prostate cancer). The location of my cancer means brachytherapy is not as likely to be effective. So my even though he is a skilled surgeon, my urologist recommended the external beam radiation.
I didn’t just take his word for it
Naturally, it seemed as if taking the prostate out would be a more certain way to get rid of the cancer. Just as naturally, it seemed like surgery with unpleasant possible side effects was something I wanted to avoid. So I wanted to make the smartest decision possible.
I asked my friend the doctor from Tufts Medical School to refer me to the best urologist in Boston. I shared my test results with that urologist and spent quite a while on the phone discussing the pros and cons of surgery vs. radiation.
I also met with a radiation oncologist, a specialist in treating cancer with radiation. I asked him a whole lot of questions about the cure rate for external radiation and what was the best choice in my case. I thought it was useful to contrast the responses from my original urologist, the radiation expert, and the second opinion. Basically, everyone agreed that the external radiation was highly likely to cure the cancer and far less likely to have serious side effects. When the surgeon and the radiation expert are both recommending radiation, you’re probably better off with radiation.
The miracle of external beam radiation
I learned a little about how external beam radiation is delivered and there’s some awesome math involved. (I promise, you won’t have to do any math to understand this, you’ll just be able to appreciate some math.)
Let’s start with tomography (the word comes from the Greek tomos meaning slice or section and graphia meaning writing or drawing). The T in a CAT scan stands for tomography. The electrical engineer Godfrey Hounsfield figured out he could use tomography for three-dimensional imaging, and that invention won him the Nobel Prize in Medicine and a knighthood.
What Hounsfield realized is that if you shot X-rays through an object rotating through every possible angle and collected the data about how much energy was blocked or passed through the object at each angle, that total collection of data was sufficient to generate a cross-section of the object. That’s how a CAT scan can compile a bunch of data from X-rays shot through your body at different angles and generate a picture of a “slice,” a cross-section of your body. To turn all that data into a picture without needing hours of computation, Hounsfield used a a clever mathematical technique called a Fast Fourier Transform that a couple of guys at IBM, James Cooley and John Tukey, had figured out a few years earlier.
The key things to realize about a CAT scan (or MRI, or any of the other 3D medical imaging scanners) is that it takes data from beams shot through an object at all possible rotational angles, and then uses fancy math to turn that data into a picture of the 3D object.
Here’s where the math comes into the external radiation therapy. They first take a CAT scan of your pelvis and your prostate to get a very precise picture of where the tumors are in your prostate. They tattoo three dots on your body to calibrate the machine, so they can line it up in precisely the right place each time.
Then the radiation technicians and doctors compute a 3D “volumetric” model of the parts of your prostate and surrounding tissues that require radiation treatment.
When it’s time to get the treatment, they position you in exactly the right spot with those tattoo dots, and a machine irradiates your body with a narrow beam at a precise strength as it rotates through every possible angle. Here’s a picture of the machine.
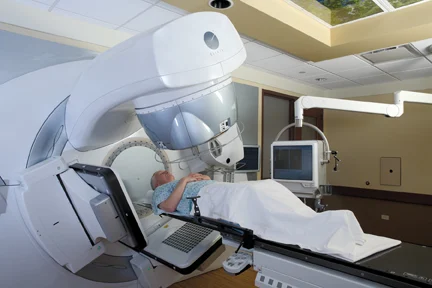
As the radiation oncologist explained this to me, I suddenly realized that this is the same mathematics involved in a CAT scan, but run in reverse!
In a CAT scan, you collect data on varying amounts of exposure from X-rays at different angles and use it to reconstruct a 3D image of a structure in the body.
In the external beam radiation therapy, you start with a 3D image of the parts of the body you want to treat with radiation and run the calculation backwards to figure out what intensity beam to use at each possible angle.
This has huge benefits. If you just shot radiation at the prostate, that radiation would also pass through whatever was in front of or behind it, possibly causing damage to other tissues as a side effect. But with this radiation therapy, called IMRT (intensity-modulated radiation therapy), the beam is much less strong at each angle. The body parts in front of or behind the beam get a far lower dose of radiation, but the targeted 3D structure in the body accumulates exactly the right amount of radiation as the modulated beam rotates completely around it.
I’ll be getting this therapy five days a week for five-and-a-half weeks starting in January, but the treatment only takes about 15 minutes a day. And the radiation will be going precisely where it’s needed to treat the cancer, with far less exposure for any of my other body parts.
Because of this mathematical and engineering miracle, I get the same very high chance of a cure as surgery, but without actually needing surgery — and with far fewer troubling side effects.
The one thing no one can answer for me
I’ve asked every doctor I’ve dealt with whether my irradiated genitals will now glow in the dark (like Rudolph’s nose). No one will give me a straight answer. That glow would be really convenient for those nighttime bathroom trips.
I guess that given the precision of the IMRT radiation treatment, any glow would be only inside my body in the exact volume treated. So nobody will ever be able to see it. I’ll just be secretly glowing inside my pants.
Trust the science. Ask the doctors a lot of questions. Don’t be afraid of medical professionals — you deserve answers, and they have the training to give them to you if ask the right questions. Make a completely informed decision with help from experts.
Wish me luck. And when you have a medical problem, I hope that the mathematical and medical technology is there to solve your problem, too.
Best of luck, Josh. My brother had a similar situation, and underwent targeted radiation therapy for multiple weeks, five days a week, a few years ago. He’s in pristine condition today. I wish the same for you. – Nancy
GOOD LUCK
I do wish you luck, as well as resilience, good humor, patience, and the love and support of your family and friends. Thanks for sharing— I’ll send this to the men in my life. I had a friend who survived it and now he’s a ski instructor (he wasn’t before), which reminds me of an old joke: “Doctor, after the surgery, will I be able to play the piano?” “Yes!” “Wonderful! I’ve always wanted to!” All the best to you, Josh.
Good luck Josh! Thanks for posting the details of your situation, especially talking to the medical professionals which is something I struggle with myself. I’m hoping that your account will help me ask more questions and get a second opinion on my own medical conditions as they arise.
It sounds like you’re in excellent hands, Josh. I hope all goes well – and, for whatever they’re worth, I’ll be sending targeted healing thoughts your way. No math involved, but lots and lots of care.
Ditto.
What a great explanation of a situation many of us could face one day. Thanks for sharing the details. I’m still in the .6 range thankfully, but will get the PSA and physical done every year to be sure it is still behaving. Here’s to a complete cure!
All the best to you, Josh, as you begin your course of treatment. Thank you for the lucid and informative article.
As always, thank you for your honest, unvarnished look at important issues. Wishing you all the best for the treatment and an easy recovery.
I went through similar radiation treatment for breast cancer in September. They were right when they said regular exercise will help with any tiredness or other side effects of the radiation. I focused on healthy eating and walking every day and I think it made a huge difference — no problems at all. Regardless of size and type, a cancer diagnosis rocks your world. I am so thankful for medical technology. I wish you all the best.
Best wishes Josh. I’ve read your column for years, learned a lot, and enjoyed hearing from you.
Reading this, I can see exactly where I got the humor and scientific curiosity with which I’ve greeted my own big scary medical problems. Sending lots of love. I hope the radiation knocks those lesions on their butts.
Josh, thank you for sharing this. I hope you write more about your experiences. Personal stories, well written, will help more men overcome fear and shame and discuss their health more openly. You’re helping save lives. Good luck.
Your intelligence, humor, and empathy shine through as always, Josh. Sending good thoughts your way.
Wish you all the best Josh, and I share the sentiment and gratitude for you sharing your experience (and without BS!).
I admire your courage, forthrightness, and intelligence. I look forward to hearing about a positive outcome.
Bon chance Josh. As always, you offer thoughtful information that doesn’t shy away from uncomfortable issues with a sardonic sense of humour. My best to you on your treatment journey.
Best wishes for a perfect outcome!
Your article is an early holiday gift to every man reading it. Thank you and best wishes.
Josh, I’m sorry to learn of your prostate cancer diagnosis. I know what a gut punch that can be as I went through the same ordeal 25 years ago. With your sharp, inquiring mind and strong constitution I expect you’ll easily conquer the Beast; it doesn’t have a chance!
By the way, I asked a “friend” you recently introduced me to to write an appropriate haiku. Here ‘tis –
Radiant beams of hope
Josh’s strength will conquer cancer
Victory awaits
Break a leg!
Tom
Excellent, fitting haiku
Thank you for completely ignoring the taboos and the cloak of embarrassment around this issue.
That was exactly my intention.
Good luck, Josh. At the moment I’m in the airport returning from a visit with two different friends with two other cancers. Wishing you success in the journey.
Sending more than enough good juju your way so you’ll sail through this adventure with juju to spare (to pass on to others).
Good luck Josh and all the best!
Thank you, Josh, for an informative post which I will share with men in my life. Your usual wit and humor shine through this very serious topic. I’m so sorry to hear you need to go through this treatment, but wish you the very best possible results.
Thanks for posting. You are not alone and that is why I support Movember for men’s health. Please support Movember and become a fund raiser or donation.
Very well researched and explained as always, Josh. I have been doing Active Surveillance since 2019. Can I add two things? 1) Anyone with prostate cancer might consider joining a support group. I belong to http://www.ancan.org, they have different groups for folks on different stages of their cancer journey. It’s free and the men there are awesome! 2) As the patient, you are in charge of what treatments you get or refuse to get, not the Doctor. We need to do our own homework, as Josh did. Doctors make mistakes, mine was explaining treatment options that made no sense to me, then we realized he had the wrong report. This is really important, thank you for sharing. I will be praying for a healthy outcome for you.
Sending best wishes, Josh. I am in active surveillance myself so I appreciate you demystifying the treatments for me. Hope you have a wonderful holiday season nonetheless.
My best wishes to you Josh from over here in the UK. The more men who talk openly about prostate cancer, the more men who will seek medical advice if they’re worried. I’m proud of you for speaking out and I wish to all the best for your treatment & recovery.
You appear to have the technology and medical expertise in hand, so I’ll send all good thoughts and blessings.
Josh, thank you so much for courageously sharing this thoughtful piece. I am saving for future reference, though I hope I will never need it.
And l want you to know that, glowing or not, you definitely have ‘em!
I suspect you’ll have this disease by them, too. Sending you positive energy and wishing you good luck!
Good luck Josh.
I had the same diagnosis in 2003 with the same Gleason score. I also had external beam radiation and achieved full remission. Today, they use even more sophisticated methods for the radiation than they had in 2003, so your chances are even better than mine were. The only thing you need to be concerned about is you might have to wear lead underwear because sometimes you glow so brightly your package shows right through your pants and you get all kinds of comments. Which reminds me of a joke:
A nurse coming on for her shift receives a report from the nurse on duty that the man in room 101 has the word “Swan” tattooed on his penis. The nurse says she has to see this and heads for the room. She returns a bit later and the other nurse asks her if she saw the tattoo. The second nurse says she did, but it doesn’t say “Swan.” It actually says . . . . . . “Saskatchewan.” Best wishes.
Good luck Josh. You’ve again provided value to readers with your clear explanation. Love the math as always. Thank you.
As a long-time reader of your blog, I appreciate you sharing this and wish you the best as you continue your treatment and recovery!
Wishing you very well with a smooth and complete recovery!
Good luck Josh, and an excellent article. I’m going through exactly the same journey as you (with some minor variations) in England. I started radiotherapy on 1st December and finish on the 30th, with a 4-day break over Christmas, so 4 more to go. I have found the most problematic part of the process to be “preparing” and holding the full bladder and empty bowel every day so the prostate is in the same place every day. Apart from that it’s a doddle! Best of luck.
Hi Josh,
Excellent article for a layman’s and professional’s perspective.Best of luck to you(your gleason’s score is favorable).We miss our long friendship with dad.Sandy and I keep in touch with mom.
Hope this will be a better year. Marty and Sandy Bascove
Thanks, Marty. All appears to be going well. Hope the same is true for you.
My brother went through this and he’s now cancer-free. It’s a heavy burden but it’s clear you have done your research and you are taking the best course of action. I’ll be sending good thoughts your way. Your sense of humor shines through this and I have always loved that about you – and that’s no bullshit.